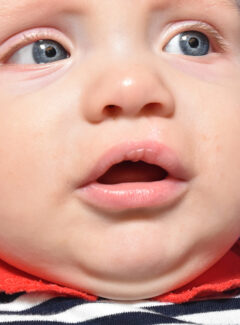
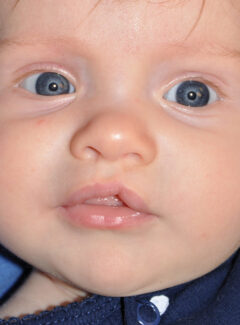
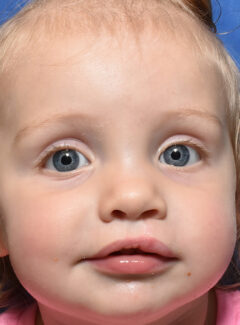
What Is a Cleft Lip and Palate?
The fourth most common birth defect, a cleft lip with or without a cleft palate is a type of facial cleft in which the facial and/or oral tissue does not properly join together during fetal development. As a result, a split or separation is left in the affected area. Dr. Eric Payne, our extensively trained craniofacial surgeon and board-certified plastic surgeon, along with our skilled multispecialty team can help correct this condition using state-of-the-art techniques. His goal is to provide optimal cosmetic and functional improvement, and to help each child achieve as normal an appearance as possible. Today’s advanced techniques make cleft lip and palate treatment more effective than ever before.
What Causes a Cleft Lip and Palate?
Approximately one out of every 700 children are born with a cleft lip with or without a cleft palate. The individual cause of a cleft lip and/or palate is often unknown, but usually is not a result of anything the mother did or did not do before or during pregnancy. However, certain medications are known to increase the risk of a cleft lip and/or palate. Genetic factors also can play a role, particularly if the cleft is a sign associated with another syndrome; in this case, the heritability will depend on the condition. Vitamin deficiencies during the first trimester of pregnancy and viral infections are also sometimes to blame for this condition. For more information, please contact our practice to ask additional questions or to schedule a consultation.
What Are the Different Types of Cleft Lip and Palate?
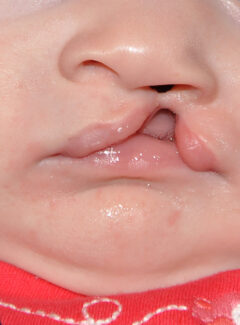
Every iteration of a cleft palate or cleft lip is unique. Still, they generally can be categorized into a handful of subsets. The types of cleft lip are:
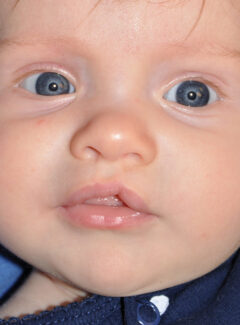
- Forme fruste or microform unilateral cleft lip: a minor cleft on one side of the upper lip
- Incomplete unilateral cleft lip: a cleft on one side of the upper lip that does not extend to the nose
- Complete unilateral cleft lip: a cleft on one side of the upper lip that does extend to the nose
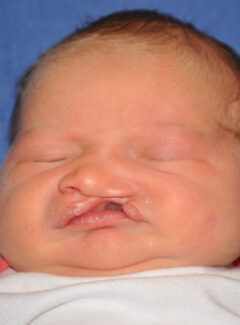
- Incomplete bilateral cleft lip: clefts on both sides of the lip that do not extend to the nose
- Complete bilateral cleft lip: clefts on both sides of the lip that do extend to the nose
Additionally, there are three main types of cleft palate, which are:
- Incomplete cleft palate: a cleft in the back of the mouth in the soft palate
- Complete cleft palate: a cleft that affects the hard and soft parts of the palate, leaving the nose and mouth cavities exposed to each other
- Submucous cleft palate: a cleft involving either the hard or the soft palate (or sometimes both), which is covered by the mucous membrane that lines the roof of the mouth
Cleft lip and palate can occur separately or together, and your child’s treatment plan will be customized to address their unique needs.
How Common Is a Cleft Lip and Cleft Palate?
The CDC estimates that each year 2,651 babies in the US alone are born with a cleft palate, and another 4,437 babies are born with a cleft lip with or without a cleft palate. In other words, the prevalence of cleft lip with or without cleft palate ranges from about 2.2 to 11.7 per 10,000 births. It is the fourth most common birth defect in the US. This condition can occur in boys and girls and individuals of all races and ethnicities; however, boys and people of Asian, Latino, and Native American ancestry are more commonly affected.
What Is a Submucous Cleft Palate?
The triad of submucous cleft palate is described as:
- Bifid uvula (a split uvula—the dangly tissue in the back of the throat)
- Palatal muscle diastasis (diastasis refers to the separation of parts normally joined together). Zona pellucida describes a clear or thin area of the soft palate where the muscles do not cross the midline
- Bony notch of the hard palate
The incidence of a submucous cleft palate is between 1:1200 and 1:6000 births per year. Approximately 10% of patients do not have a normally functioning palate due to the submucous cleft, leading to what is called velopharyngeal insufficiency. This is due to three things: a short palate, poor muscle control, and easily tired muscle or fatigue. Recurrent ear infections with otitis media (inflammation of the middle ear) can cause hearing loss in children with a submucous cleft palate.
When Do You Operate for a Submucous Cleft Palate?
There is no reason to operate on an infant solely because of the submucous cleft palate. The symptoms of poor speech and VPI are clear indications for surgical intervention when a submucous cleft is identified in a child. Usually a child is evaluated when a proper speech test can be performed at the ages four to six years old. A proper speech evaluation with a hearing test and videonasoendoscopy/videofluoroscopy should be performed to determine if surgical intervention is needed. Some infants with severe feeding issues may need to be carefully evaluated to determine the function of the soft palate and can lead to earlier surgical intervention.
When Should I Seek Cleft Lip and Palate Treatment?
Typically, a consultation can be performed at the initial diagnosis of the cleft either in-utero or within the first few days of life. Discussing your options for how to proceed with treatment can significantly ease your fears. We would like to arrange training for feeding and monitoring your baby’s progress with weight gain. The repair of the cleft lip does not depend on a specific age of your baby, but rather the overall weight and health of your child. This makes undergoing general anesthesia safer for the baby.
Typically, the ideal schedule to address a cleft lip and palate is as follows:
3 – 6 Months Old
- Cleft lip repair
- Veloplasty – soft palate repair (this is the 1st stage of a 2 part cleft palate repair; not all surgeons perform a 2 stage repair of the palate)
9 – 12 Months Old
- Single stage palatoplasty
18 – 24 Months Old
- Palatoplasty – hard palate repair (this is the 2nd stage of a two part palate repair)
- Columellar lengthening (if needed)
6 – 9 Years Old
- When the cleft side canine tooth is half developed, then we can perform alveolar bone grafting with cancellous bone. This is bone marrow from the hip made through a small incision.
After Puberty (16-18 years old)
- Lefort I advancement – upper jaw surgery that moves the upper jaw forward to allow for a proper dental occlusion so the teeth can be in proper alignment
- Rhinoplasty with or without a rib graft – final nasal reconstruction to allow for proper breathing through the nose (the deviated septum will be treated at this time)
How Is Cleft Lip and Palate Repaired?
It takes a team of specialists who are involved in treating children with this type of deformity to repair cleft lip and/or palate. Specialists include: plastic surgeon, otolaryngologist (ENT surgeon), orthodontist, dentist, speech pathologist, audiologist, and a geneticist. Two procedures generally performed for cleft lip and palate repair are nasal-alveolar molding and two-stage palatoplasty repair, both of which are highlighted below.
Nasal-Alveolar Molding
Due to the flattening of the cleft side nostril and misalignment of the alveolar segments, nasal alveolar molding is used to reshape these into a more natural shape and location. Initiating nasal-alveolar-molding (or NAM) during the first week of life is very important. Most craniofacial surgeons leave this up to an orthodontist or dentist to decide and initiate. But our experience and training has shown this can be started at the initial visit. Dental impressions will be obtained to create the device, with emphasis on molding the shape of the nose and alveolar units. Starting this therapy early greatly increases the chances of obtaining a successful result. Delays in meeting with an orthodontist or dentist should not be tolerated.
NAM treatment requires a commitment on the part of the parents and the surgeon. Visits in the office are required on a weekly to every other week basis. Twice daily removal with cleaning and repositioning of the NAM device is required. Taping of the upper lip to stretch the lip skin and muscle is also performed with the NAM. This is done by the parents at home and become part of the normal routine, just like feedings and changing the diaper. The child should become accustomed to the device much like a pacifier and may fuss more when the device is removed. The child may also find it easier to feed in instances where the cleft in the hard palate is present.
Nasal-Alveolar Molding Instructions
Two-Stage Palatoplasty Repair
The early two-stage repair has been controversial because a study has not been designed that compares long-term outcomes between single stage and early two stage repair. Early two-stage repair is defined as completing both stages of the palatoplasty before the child reaches two years of age. In the past, surgeons have performed a late two-stage repair with limited success, hoping that mid-facial development would be improved. This, however, resulted in very poor speech. Early two-stage repair avoids the poor speech outcomes by repairing the hard palate before two years of age. The potential to achieve better speech results and avoid mid-face development issues are, in theory, possible. This is due to the very early repair of the soft palate where the muscles are realigned to a normal anatomic position for phonation and velopharyngeal competency. Allowing the hard palate to continue to develop without a scar until the child is at least 18 months old may help to reduce the mid-face deficiency.
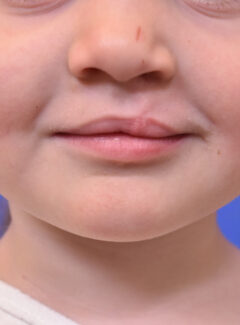
Will My Child Have a Cleft Lip and Palate Scar?
Depending on the severity of the cleft lip and/or palate, there will likely be a scar once treatment is complete. This mark, which can affect just the mouth or the mouth and the nose, is a “visible difference.” A cleft lip scar is nothing to be ashamed of; however, it can cause self-esteem issues in some individuals. There are many options available to address this concern, including surgical cleft lip revision. If Dr. Payne is performing your primary cleft lip surgery, he will make every effort to provide an aesthetically appealing outcome. If you are seeking a revision to minimize the appearance of a scar, Dr. Payne will customize a treatment plan that can optimize your results.
Learn More About Cleft Lip and Palate
Parents often have many questions about cleft lip and palate and what the best way is to care for a child with one or both of these defects. Dr. Payne has answered some of the most common questions below, and you are welcome to contact our practice for additional information.
Did I do anything wrong to cause my child to have a cleft lip and palate?
Some parents—and especially mothers—feel guilty about a child born with a cleft. Aside from avoiding the risk factors, such as smoking and alcohol, there is little you can do to predict if a child will be born with a birth defect. Some parents believe it is God punishing them for sins they committed. This is the furthest thing from the truth, and cleft children are born into all kinds of families; rich or poor, black, white, Asian, Hispanic, religious or atheist. The saddest part is when children are abandoned because of their deformities. This happens all over the world because people believe these children are cursed or useless to society. When you see a young teenage girl or boy who has gone through so many surgeries and taunting from schoolmates, you will see a strong-willed, determined young adult who is amazingly beautiful.
If I have a cleft lip and/or palate, what are the chances my baby will have one?
First, let’s look at the general population frequency of cleft lip and palate and isolated cleft lip alone. The frequency of a cleft lip/palate defect in the general population is about 0.1% compared to a cleft palate alone presenting in 0.04% of the population. If a parent has an affected child and no other affected relatives, the risk of another baby being affected with a cleft lip/palate is 4%, with a 2% risk for cleft palate alone to occur in the new baby. If there is an affected relative, the risk for having an isolated cleft palate in the next baby increases to 7%.
If two children are affected but the parents are unaffected, then the risk of the next baby being born with a cleft lip/palate is 9% with the isolated cleft palate risk at 1%. If one of the parents has a cleft lip or palate, the risk of having a child with cleft lip/palate is 4%, and the risk for isolated cleft palate is 6%. If a child is affected and one of the parents also has a cleft, then the risk of the next child having a cleft lip/palate goes up to 17%, and isolated cleft palate risk goes to 15%.
What imaging studies are available, and when should the study be ordered for clefting prenatally?
Commonly, high resolution 3D Ultrasound detects cleft lips and palates and with greater rates in bilateral clefts. MRI can also be used for prenatal evaluation but the cost has not shown a benefit. Typically, a screening ultrasound can and will detect a cleft lip more commonly than a cleft palate. Screening ultrasound is performed at 18 weeks gestation.
What feeding recommendations should you make to improve oral intake after cleft lip repair?
Breastfeeding can be—and should be—encouraged after cleft lip repair, because there is no increased risk of disrupting the repair and there is an increase in body weight of babies at six weeks after surgery. Typically breastfeeding is not always adequate to supply enough milk per feeding, therefore giving some formula along with the breast milk will be necessary. If a cleft palate is also repaired, using syringe feeds may be necessary for the first few days due to the baby’s discomfort and pain when using a nipple with feeding from a bottle.
What if there are feeding issues?
A cleft lip alone does not typically cause difficulty with feeding, but a cleft palate will not allow for your baby to generate enough suction to feed normally. There are several types of nipples that can assist your baby in achieving as much volume in each feeding as possible. Three of the most popular nipples are the Haberman nipple, the Pigeon nipple, and the Dr. Brown’s nipple specialty feeding system. We also recommend using a vented bottle, as this will help decrease the amount of air swallowed with the feeding.
Why does my child need to see an ear-nose-throat (ENT) surgeon?
Hearing is a very important aspect of a cleft palate. To prevent hearing loss in patients with cleft palate, your child may need ear tubes placed by an ENT surgeon at the time of the repair. This prevents buildup of fluid behind the eardrum due to a dysfunctional drainage by the Eustachian tube.
Contact Our Practice
We understand you may have more questions about cleft lip and palate and how these conditions can be corrected. Our skilled medical team can provide additional and more personalized information at the time of a consultation. Simply contact our office online or by telephone today.